Let’s Talk about Bias in Healthcare: Experiences from an Interactive Interprofessional Student Seminar
DOI:
https://doi.org/10.5195/ijms.2025.2457Keywords:
interprofessional education, implicit bias education, Bias in medicine, structural competency, racial bias, health professions education, undergraduate health educationAbstract
Background: Education to increase awareness of the impact of bias in healthcare should be included in all health professions training programs. This report describes the implementation and outcomes of an interactive, interprofessional pilot seminar on racial bias in healthcare for health professions students.
Methods: Forty students across the University of Nebraska Medical Center’s six health profession colleges participated in a 3-part, 1-hour seminar, including a video vignette depicting examples of bias in the hospital, facilitated interprofessional small group discussions, and interaction with a health equity expert panel. We analyzed the results of participants’ Ethnic Perspective-Taking (EP) and Implicit Bias Knowledge scale (IBKS) scores before and after the seminar.
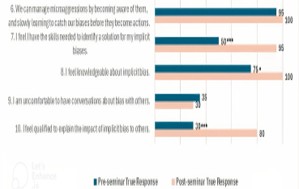
Results: There was a statistically significant increase (p<0.001) in the average post-seminar EP scores (30.6 post-seminar vs 27.8 pre-seminar). For the adapted IBKS, there were significant improvements in participant knowledge, skills to identify, and ability to explain the impact of implicit biases (p<0.05). Participants highlighted the importance of including education about bias in healthcare training, and some suggested mandatory education. All facilitators agreed that learners gained a deeper appreciation for the effect of bias and racism on health outcomes and participants understood how bias and racism affect patient care and clinician experience after the seminar.
Conclusion: Health professions training often lacks integrated interprofessional and health equity education. This seminar addresses both, engaging community voices without heavy resources. Despite low participation, results show the benefits of interactive sessions on health equity, helping students grasp their role in equitable care and influencing future practice.
References
Disparities: Where Do We Go from Here? Perm J. 2011;15(2):71–8.
Marcelin JR, Siraj DS, Victor R, Kotadia S, Maldonado YA. The Impact of Unconscious Bias in Healthcare: How to Recognize and Mitigate It. J Infect Dis. 2019;220(Supplement_2):S62–73.
Sabin JA, Rivara FP, Greenwald AG. Physician Implicit Attitudes and Stereotypes About Race and Quality of Medical Care. Med Care. 2008;46(7):678–85.
Moskowitz GB, Stone J, Childs A. Implicit Stereotyping and Medical Decisions: Unconscious Stereotype Activation in Practitioners’ Thoughts About African Americans. Am J Public Health. 2012;102(5):996–1001.
Power-Hays A, McGann PT. When Actions Speak Louder Than Words — Racism and Sickle Cell Disease. N Engl J Med. 2020;383(20):1902–3.
Oliver MN, Wells KM, Joy-Gaba JA, Hawkins CB, Nosek BA. Do Physicians’ Implicit Views of African Americans Affect Clinical Decision Making?J Am Board Fam Med. 2014;27(2):177–88.
Green AR, Carney DR, Pallin DJ, Ngo LH, Raymond KL, Iezzoni LI, et al. Implicit Bias among Physicians and its Prediction of Thrombolysis Decisions for Black and White Patients. J Gen Intern Med. 2007;22(9):1231–8.
Hoffman KM, Trawalter S, Axt JR, Oliver MN. Racial bias in pain assessment and treatment recommendations, and false beliefs about biological differences between blacks and whites. Proc Natl Acad Sci USA. 2016;113(16):4296–301.
LCME. Standards, Publications, & Notification Forms. Available from: https://lcme.org/publications/. Cited Aug 23, 2023.
Merritt R, Rougas S. Multidisciplinary approach to structural competency teaching. Med Educ. 2018;52(11):1191–2.
Benoit LJ, Travis C, Swan Sein A, Quiah SC, Amiel J, Gowda D. Toward a Bias-Free and Inclusive Medical Curriculum: Development and Implementation of Student-Initiated Guidelines and Monitoring Mechanisms at One Institution. Acad Med. 2020;95(12S):S145–9.
Khazanchi R, Keeler H, Strong S, Lyden ER, Davis P, Grant BK, et al. Building structural competency through community engagement. Clin Teach. 2021;18(5):535–41.
Perdomo J, Tolliver D, Hsu H, He Y, Nash KA, Donatelli S, et al. Health Equity Rounds: An Interdisciplinary Case Conference to Address Implicit Bias and Structural Racism for Faculty and Trainees. MedEdPORTAL. 2019;10858.
Hardeman RR, Burgess D, Murphy K, Satin DJ, Nielsen J, Potter TM, et al. Developing a Medical School Curriculum on Racism: Multidisciplinary, Multiracial Conversations Informed by Public Health Critical Race Praxis (PHCRP). Ethn Dis. 2018;28(Supp 1):271.
Sabato E, Owens J, Mauro AM, Findley P, Lamba S, Fenesy K. Integrating Social Determinants of Health into Dental Curricula: An Interprofessional Approach. J Dent Educ. 2018;82(3):237–45.
Neff J, Holmes SM, Knight KR, Strong S, Thompson-Lastad A, McGuinness C, et al. Structural Competency: Curriculum for Medical Students, Residents, and Interprofessional Teams on the Structural Factors That Produce Health Disparities. MedEdPORTAL. 2020;16:10888.
Cox C, Hatfield T, Moxey J, Fritz Z. Creating and administering video vignettes for a study examining the communication of diagnostic uncertainty: methodological insights to improve accessibility for researchers and participants. BMC Med Res Methodol. 2023;23(1):296.
Hillen MA, Van Vliet LM, De Haes HCJM, Smets EMA. Developing and administering scripted video vignettes for experimental research of patient–provider communication. Patient Educ Couns. 2013;91(3):295–309.
Labrie N, Kunneman M, Van Veenendaal N, Van Kempen A, Van Vliet L. Using expert opinion rounds to develop valid and realistic manipulations for experimental video-vignette research: Results from a study on clinicians’ (un)reasonable argumentative support for treatment decisions in neonatal care. Patient Educ Couns. 2023;112:107715.
Stacey D, Brière N, Robitaille H, Fraser K, Desroches S, Légaré F. A systematic process for creating and appraising clinical vignettes to illustrate interprofessional shared decision making. J Interprof Care 2014;28(5):453–9.
Interprofessional Education Collaborative. Core Competencies for Interprofessional Collaborative practice: 2016 Update. Available from: https://ipec.memberclicks.net/assets/2016-Update.pdf. Last updated 2016; cited Sept, 2023.
thinkMOTION. Racial Bias (captioned). Available from: https://vimeo.com/691129770/6410d11479. Last updated Mar 22, 2022; cited Mar 22, 2022.
Galinsky AD, Ku G, Wang CS. Perspective-Taking and Self-Other Overlap: Fostering Social Bonds and Facilitating Social Coordination. GPIR. 2005;8(2):109–24.
Todd AR, Galinsky AD. Perspective-Taking as a Strategy for Improving Intergroup Relations: Evidence, Mechanisms, and Qualifications: Perspective-Taking and Intergroup Relations. Soc Personal Psychol Compass. 2014;8(7):374–87.
Liu FF, Coifman J, McRee E, Stone J, Law A, Gaias L, et al. A Brief Online Implicit Bias Intervention for School Mental Health Clinicians.Int J Environ Res Public Health. 2022;19(2):679.
Todd AR, Bodenhausen GV, Richeson JA, Galinsky AD. Perspective taking combats automatic expressions of racial bias.J Pers Soc Psychol. 2011;100(6):1027–42.
Stone J, Moskowitz GB. Non-conscious bias in medical decision making: what can be done to reduce it?: Non-conscious bias in medical decision making. Med Educ. 2011;45(8):768–76.
Wang YW, Davidson MM, Yakushko OF, Savoy HB, Tan JA, Bleier JK. The Scale of Ethnocultural Empathy: Development, validation, and reliability. J Couns Psychol. 2003;50(2):221–34.
Fix RL. Justice Is Not Blind: A Preliminary Evaluation of an Implicit Bias Training for Justice Professionals. Race Soc Probl. 2020;12(4):362–74.
Braun V, Clarke V. Thematic analysis. In: Cooper H, Camic PM, Long DL, Panter AT, Rindskopf D, Sher KJ, editors. APA handbook of research methods in psychology, Vol 2: Research designs: Quantitative, qualitative, neuropsychological, and biological. Washington: American Psychological Association; 2012;57–71.
Sun M, Oliwa T, Peek ME, Tung EL. Negative Patient Descriptors: Documenting Racial Bias In The Electronic Health Record. Health Aff (Millwood). 2022;41(2):203–11.
Park J, Saha S, Chee B, Taylor J, Beach MC. Physician Use of Stigmatizing Language in Patient Medical Records. JAMA Netw Open. 2021;4(7):e2117052.
Qin E, Seeds A, Wallingford A, Copley M, Humbert A, Junn C, et al. Transmission of Bias in the Medical Record Among Physical Medicine and Rehabilitation Trainees. Am J Phys Med Rehabil. 2023;102(8):e106–11.
P. Goddu A, O’Conor KJ, Lanzkron S, Saheed MO, Saha S, Peek ME, et al. Do Words Matter? Stigmatizing Language and the Transmission of Bias in the Medical Record. J Gen Intern Med. 2018;33(5):685–91.
University of Nebraska Medical Center Academic Affairs. Interprofessional Education. Available from: https://www.unmc.edu/academicaffairs/educational/ipe/index.html. Cited 2024 Oct 26.
Stumbar S, Lage O, Whisenant EB, Brown DR. Developing the Community Engaged Physician: Medical Students Reflect on a Household Visit Curriculum. Cureus. 2020;12(11):e11593.
Julian Z, Mengesha B, McLemore MR, Steinauer J. Community-Engaged Curriculum Development in Sexual and Reproductive Health Equity: Structures and Self. Obstet Gynecol. 2021;137(4):723–7.
Bromage B, Encandela JA, Cranford M, Diaz E, Williamson B, Spell VT, et al. Understanding Health Disparities Through the Eyes of Community Members: a Structural Competency Education Intervention. Acad Psychiatry. 2019;43(2):244–7.
Meleis AI. Interprofessional Education: A Summary of Reports and Barriers to Recommendations: Interprofessional Education. J Nurs Scholarch. 2016;48(1):106–12.
Khazanchi R, Keeler H, Marcelin JR. Out of the Ivory Tower: Successes From a Community-Engaged Structural Competency Curriculum. Acad Med. 2021;96(4):482–482.
Published
How to Cite
Issue
Section
Categories
License
Copyright (c) 2024 Mckenzie P. Rowe, Nancy B. Tahmo, Opeoluwa O. Oyewole, Keyonna M. King, Teresa M. Cochran, Yun Saksena, Carolyn T. Williamson, Rev. Portia A. Cavitt, Sherrita A. Strong, Michael D. Griffin, Timothy C. Guetterman, Jasmine R. Marcelin

This work is licensed under a Creative Commons Attribution 4.0 International License.
Authors who publish with this journal agree to the following terms:
- The Author retains copyright in the Work, where the term “Work” shall include all digital objects that may result in subsequent electronic publication or distribution.
- Upon acceptance of the Work, the author shall grant to the Publisher the right of first publication of the Work.
- The Author shall grant to the Publisher and its agents the nonexclusive perpetual right and license to publish, archive, and make accessible the Work in whole or in part in all forms of media now or hereafter known under a Creative Commons Attribution 4.0 International License or its equivalent, which, for the avoidance of doubt, allows others to copy, distribute, and transmit the Work under the following conditions:
- Attribution—other users must attribute the Work in the manner specified by the author as indicated on the journal Web site; with the understanding that the above condition can be waived with permission from the Author and that where the Work or any of its elements is in the public domain under applicable law, that status is in no way affected by the license.
- The Author is able to enter into separate, additional contractual arrangements for the nonexclusive distribution of the journal's published version of the Work (e.g., post it to an institutional repository or publish it in a book), as long as there is provided in the document an acknowledgment of its initial publication in this journal.
- Authors are permitted and encouraged to post online a prepublication manuscript (but not the Publisher’s final formatted PDF version of the Work) in institutional repositories or on their Websites prior to and during the submission process, as it can lead to productive exchanges, as well as earlier and greater citation of published work. Any such posting made before acceptance and publication of the Work shall be updated upon publication to include a reference to the Publisher-assigned DOI (Digital Object Identifier) and a link to the online abstract for the final published Work in the Journal.
- Upon Publisher’s request, the Author agrees to furnish promptly to Publisher, at the Author’s own expense, written evidence of the permissions, licenses, and consents for use of third-party material included within the Work, except as determined by Publisher to be covered by the principles of Fair Use.
- The Author represents and warrants that:
- the Work is the Author’s original work;
- the Author has not transferred, and will not transfer, exclusive rights in the Work to any third party;
- the Work is not pending review or under consideration by another publisher;
- the Work has not previously been published;
- the Work contains no misrepresentation or infringement of the Work or property of other authors or third parties; and
- the Work contains no libel, invasion of privacy, or other unlawful matter.
- The Author agrees to indemnify and hold Publisher harmless from the Author’s breach of the representations and warranties contained in Paragraph 6 above, as well as any claim or proceeding relating to Publisher’s use and publication of any content contained in the Work, including third-party content.
Enforcement of copyright
The IJMS takes the protection of copyright very seriously.
If the IJMS discovers that you have used its copyright materials in contravention of the license above, the IJMS may bring legal proceedings against you seeking reparation and an injunction to stop you using those materials. You could also be ordered to pay legal costs.
If you become aware of any use of the IJMS' copyright materials that contravenes or may contravene the license above, please report this by email to contact@ijms.org
Infringing material
If you become aware of any material on the website that you believe infringes your or any other person's copyright, please report this by email to contact@ijms.org







