Guerrilla Eye Service mission.
Francisco J. Bonilla-Escobar12
doi: http://dx.doi.org/10.5195/ijms.2017.47
Volume 5, Number 3: 117-120
Received 26 05 2017: Accepted 23 06 2017
Evan L. Waxman, MD, PhD is a passionate doctor and educator who has spent part of his life volunteering to prevent blindness especially where poverty and lack of opportunities are prevalent.
He studied medicine and obtained a Ph.D. in basic science at Mount Sinai Medical School, NY. He graduated in ophthalmology at the UC Davis Medical Center and is the Director of the Ophthalmology service at the Eye Center at UPMC Mercy Hospital and the Residency Program of Ophthalmology at the University of Pittsburgh. He is the creator of the Guerrilla Eye Service, a unique 10-year-old program created to serve the underserved communities in Pittsburgh with an army of medical students, residents and faculty from the same University.1
I remember being asked when I was interviewing for medical school, why do you want to be a doctor.1 It's something that anybody can say, I became a doctor because I want to help people.
I found that ophthalmology is a great blend of medicine and surgery. In ophthalmology, we work on patients' quality of life. Ophthalmology has the best tools and gadgets of any of the fields, and it's a great research field as well. There are many important questions in ophthalmology that haven't been answered yet and seems like you should be able to answer them.
I would find it hard to point out anything spectacular. Quite frankly, there are things I am proud of. I am proud to be faculty at the University of Pittsburgh and have the opportunity to offer the multiplier effect of teaching. I get to teach medical students and residents who in turn impact this knowledge on other people, their peers, and patients. I am focused on this issue of losing your way in medicine, and forgetting that it is all about helping people, and I'm really pleased to have had the opportunity to create the Guerilla Eye Services. This is an outreach program we have, where we take our medical students and residents out to places where patients are not getting eye care, out of primary care sites and we provide it. We do a good job for the patients, while we are out there, and I am proud of that.
Having grown up as a white suburban middle-class American, I consider myself privileged to have been provided for by my parents. I realized that many were not so privileged. Circumstances such as lack of money, lack of transportation, lack of time to visit a doctor prevent such people from getting eye care. Many people go into medical practice with the hope of helping people but along the way as the stresses in medical school become apparent, as you realize that they are other components to practicing medicine, like billing and coding, and charting, and all the parts of medicine that nobody really loves, you start to lose track of the “I want to help people” part. Not everybody goes through this phase. I think as important as what we do for patients in GES is what we do for the medical students and residents that participate. We get into medicine to help people but then we get burn-out and forgot that idea. In the GES, they are learning some ophthalmology, sure, but I think that community work like that provides an antidote to that cynicism.
It is a sort of commando eye squad where we take medical students and residents to primary care sites where patients can't access eye care. We bring portable equipment and we set up a complete eye examination room – and the team of medical students and residents unpack the equipment into the space we are going to use. We set everything up, see a dozen patients or so, and then we pack up the equipment back up, put it back in the van and call it a day. We don't do screening; we do complete front to back eye care. We become the eye patients' doctor. We also leave our medical notes in the clinics. This makes it easier for them to know which patient has diabetic retinopathy and they know that's a patient that needs extra attention.
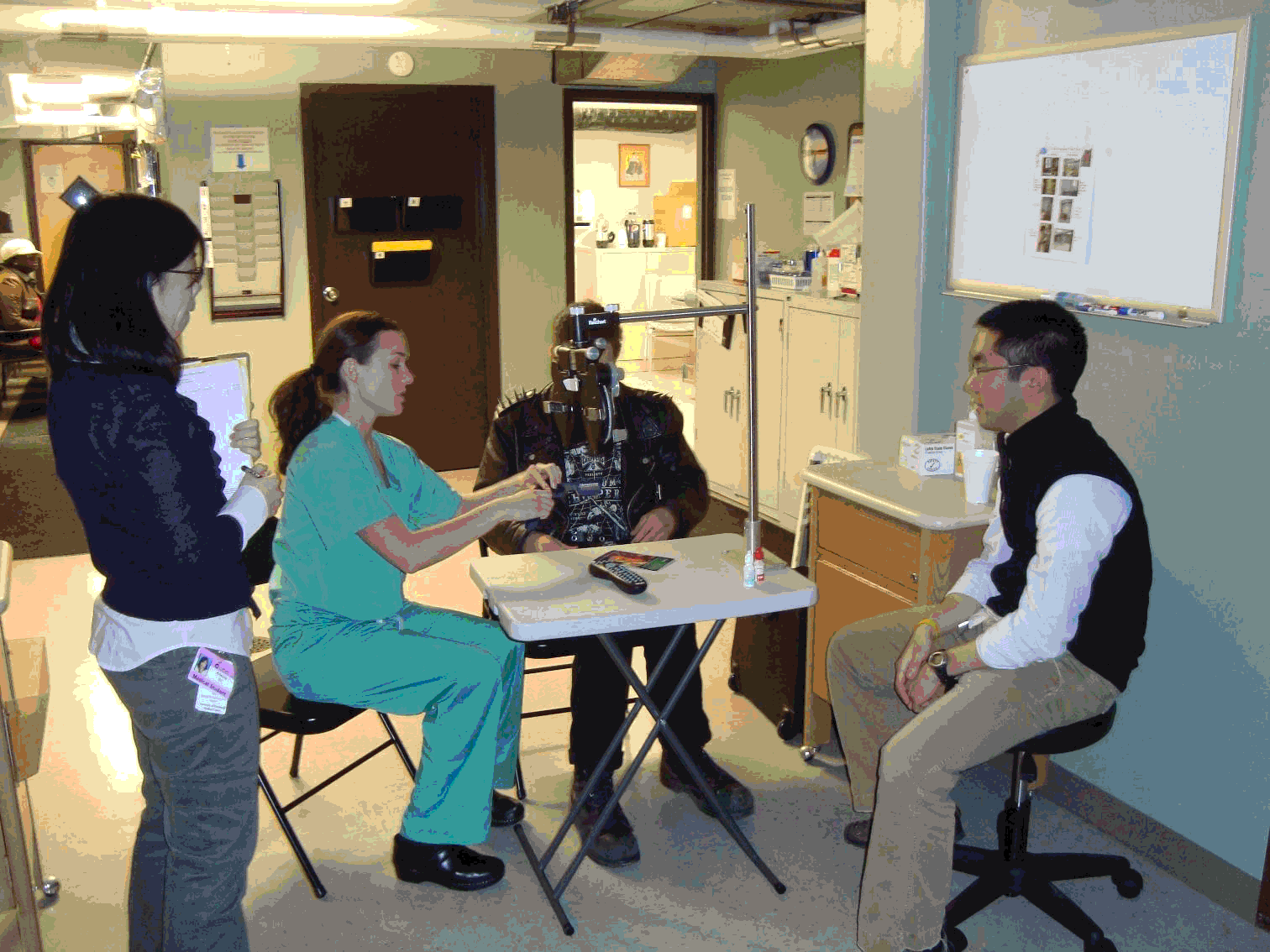
We've got medical students with a lot of energy, the healthcare need of the low-resource communities, and the idea that we should be doing mission trips, not only to serve people over the US, but to help the people in our backyard. This is what Guerrilla Eye Service entails, missions into our own backyard, to provide eye care for people who wouldn't otherwise get it (Figure 1).
Figure 1.Guerrilla Eye Service mission.

The corny name was conceived from the idea that we need to travel light with a group of people, unpack, set-up, save sight, be the patients' eye doctor on site, and get back. It's like a commando team; a military organization.
It has been such a long time ago. I remember ups and downs we've had along the way. I remember the time I showed up for the Guerrilla Eyes Service and there were no students, and so I had the pleasure of unpacking and setting up the equipment myself, seeing the patients myself and packing it up myself. I also remember being down in Green County admitting a patient who had a retinal detachment and feeling “wow, it's great we are here”, but became surprised when the patient worried over the issue of traveling and paying medical doctors in Pittsburgh to fix his retina than he was worried about his vision itself. That was eye opening (Figure 2).
There are always those people who are extraordinarily grateful. And they shouldn't have to be. They think of us, the residents, and the medical students, as their eye doctors and this is pretty satisfying.
It has become a lot easier. At first, we did not have a van and so all the equipment lived at my house. We had to pack my car up before the mission and then I unpack it at 10 or 11 PM when I got home. At the time, I was the only faculty that went on three missions a month, and it was only like four years ago, or so, that one of the medical students said, “You know, it's time to get other faculty involved”. So they started recruiting some of the other faculty. The UPMC Mercy Hospital was kind enough to get us a van that helped us with the work, and the equipment is now living there. It's been a relief and a big change.
GES is becoming more of a student-run clinic/organization with more people getting involved which I think is fantastic. Now the students are making it happen. We have trainees at GES, students from all four years of medical school and residents from each year of training. We also have fellows that come to visit sometimes. It is exciting to see the senior medical students teach the junior ones who end up growing in ranks at GES to become team leaders. And now, in the institutional memory, I no longer have to show up at the mission just to show everybody how to set the equipment up. The senior students are teaching the junior students and then they teach the next group and I become less essential to the project. I'm so proud of that.
In each mission, the GES takes care of 10 patients in average. There are three missions per month, therefore per year are estimated a total of 360 patients. In ten years, that means more than 3000 patients.
My expectation is that GES continues to grow and attend to more clinics to reach as many people as possible. Even with our three missions a month, we haven't actually stamped out all the blindness in Western Pennsylvania, yet. With the help of the GES Reconnaissance Program, the nonmydriatic retinal cameras are able to detect diabetic retinopathy among diabetic patients early and to reach everybody in their own primary care clinic.
I realize that in addition to delivering eye care, we should also create a kit, or publicize the model. We would like to see GES go national.
The standard of eye care in the United States is that every person with diabetes gets a dilated eye exam once a year but people don't do that. The prevalence of any retinopathy in persons with diabetes is 35%, while proliferative (vision-threatening) retinopathy is 7%.2 However, retinopathy rates are higher among people with lower socioeconomic status or African-descendent people.3 People who do not have challenges with their vision do not see any reason to get checked out. Someone might be seeing fine but have a lot of diabetic retinopathy which is easier to treat when detected early before such a person loses their eyesight. We need to get the word out. So, mobility, transportation, geography, finances, and education are big barriers.4
If there is going to be a next step for GES, it would be to branch out and get out kits that people can use to set up anywhere. There is a spin-off from Guerrilla Eye Service to Guerrilla Eye Service Mobile and the Guerrilla Eye Service Reconnaissance (Recon).
The GES Mobile are the missions, and the GES Recon is where we're taking nonmydriatic retinal cameras to take photos in primary care offices. Therefore, instead of trying to do the impossible, we just get every patient in to eye doctor who doesn't want to go, we'll just work on the ones who have abnormal photos.
There was too much more that we could do with GES Mobile. Three missions a month was about the maximum we could get attendings, residents, and medical students out. This wasn't enough. And since I can't live at every one of these clinics, the next best thing is to have a reconnaissance program. Have the cameras out there so that the primary care team can take the images and report back.
The first camera was installed 6 years ago, but the GES Recon program started in 2015. We brainstormed a bunch of ideas and discovered that this is a GES spin-off that should be different from the mobile unit. Today we have fifteen cameras with more coming.
Pitching one camera on one foundation and seeing that it works helped in spreading the word. Some clinics now make a call and they said; “Well, can we have that over here?”. The cameras were borrowed between clinics, they took photos, get some numbers, identify the problem and pitch to fundraise for their own camera. That's how we've grown.
For our future steps, we have two models – GES Mobile and the GES Recon. The Recon program is interesting because it gives us room to follow up on patients that need to see an eye doctor but fail to do so.
I believe that just as much as the academic mission concerns teaching, and contacts patient care, they are also to reach out to communities and work with and for them.
In terms of research, in my Ph.D. in biomedical sciences, I studied proteins. And that's kind of research. I have come to realize that although we have treatment for a lot of things, it still doesn't get to the people. This is just as important if you have the best treatment in the world and it doesn't get to the people who need it for one reason or another, what good is that? This calls for research too.
The diversity I see in people is incredible. The diversity in pathology I see is, something that I can't imagine I'd see in community practice. And I guess as importantly as each and every one of those things individually, I get to see the synergy in all of them, I get to see how teaching medical students really meshes with teaching residents. And I get to see how teaching residents and medical students meshes with taking care of the undeserved. And I get to see how taking care of the undeserved meshes with delivery of care research. And it's just an incredibly rich experience and the best job in the world.
Figure 2.Dr. Waxman helping to unpack equipment for the GES mission.

Remember why you're in it, that's the most important thing. You are here to take care of people. If you forget that in this stage, you are lost. If you remember that you're here to take care of people, to help people and use that as your guide for what to do, you're going to love what you do. It's not going to matter what the Medicare regulation there is or the documentation burden you have, none of that matters if you come to work and remember why you are here.
The words ‘patient-centered’ has been repeated so many times recently that they start to lose meaning and that's where we need to be. We need to be patient-centered. We are in the business to help people, we've got to be not patient-centered and we've got to be people centered.
He closed his interview with a clear and loud message for the medical community: Hopefully, they'll find something in this story that overlaps with their interests, so they may not be interested in eyes, or in hearing, or in gastrointestinal problems. It may not have anything to do with medicine at all, but they may realize that they have some talent, some skill, that's not getting to people who need it. And they may feel, you know I do 40-hour work week providing the skill for money, and it doesn't always feel satisfying. Maybe it would feel good to give it to some people who need it, but who wouldn't otherwise be able to get it. And like I said, that's our job. Write a good story.
Dr. Evan L. Waxman, for his generosity and charisma, and for sharing this amazing perspective about academia, research, and service.
The Author have no funding, financial relationships or conflicts of interest to disclose.
Conception and design the work/idea. Collect data/obtaining results. Analysis and interpretation of data. Write the manuscript, Critical revision of the manuscript, Approval of the final version: FJBE.
1.Fogel C, Waxman E. The Guerrilla Eye Service Reconnaissance Project – A New Model to Meet the Needs of High-Risk Populations. Sight+Sound. 2016 Fall:7.
2.Yau JW, Rogers SL, Kawasaki R, Lamoureux EL, Kowalski JW, Bek T, . Global prevalence and major risk factors of diabetic retinopathy. Diabetes Care. 2012 Mar;35(3):556–64.
3.Emerging Risk Factors Collaboration, Sarwar N, Gao P, Seshasai SR, Gobin R, Kaptoge S, . Diabetes mellitus, fasting blood glucose concentration, and risk of vascular disease: a collaborative meta-analysis of 102 prospective studies. Lancet. 2010 Jun 26;75(9733):2215–22.
4.Daskivich LP, Mangione CM. The promise of primary care-based screening for diabetic retinopathy: the devil will be in the details. Arch Intern Med. 2012 Nov 26;172(21):1678–80.
Francisco J. Bonilla-Escobar, 1 MD, MSc, University of Pittsburgh, PA, USA. Universidad del Valle, Cali, Colombia.
About the Author: Francisco J. Bonilla-Escobar is a PhD student at the Institute of Clinical Research Education at the University of Pittsburgh.
Correspondence: Francisco J. Bonilla-Escobar, Address: 1400 Locust St, Pittsburgh, PA 15219, USA. Email: fjbonillaescobar@gmail.com
Cite as: Bonilla-Escobar FJ. Fighting blindness with a Guerrilla: The Guerrilla Eye Service of Pittsburgh. Int J Med Students. 2017 Sep-Dec:5(3):117-120.
Copyright © 2017 Francisco J. Bonilla-Escobar
International Journal of Medical Students, VOLUME 5, NUMBER 3, December 2017