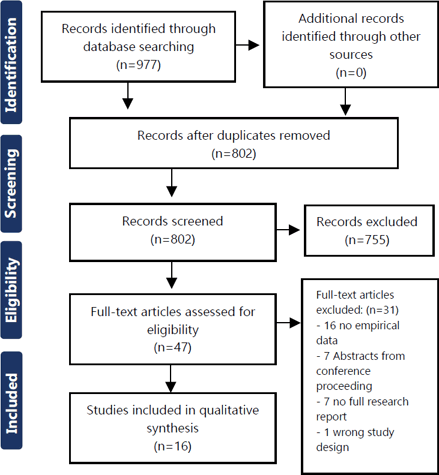
PRISMA Diagram of Article Selection Process.
Mallory A. Evans1, Eric J. James2, Misa Mi3
doi: http://dx.doi.org/10.5195/ijms.2023.1717
Volume 11, Number 1: 58-66
Received 27 09 2022; Rev-request 12 11 2022; Rev-recd 16 11 2022; Accepted 01 03 2023
ABSTRACT
Background:This review seeks to characterize existing curricular interventions implemented to develop leadership skills in undergraduate medical students at LCME-accredited medical schools and elucidate best practices for leadership curriculum development.
Methods:PRISMA guidelines were used to guide the review. Comprehensive literature searches of five databases retrieved peer-reviewed journal articles with empirical data published in English. Two phases of screening were conducted to identify studies describing leadership development curricular interventions, followed by data extraction and synthesis.
Results:Comprehensive literature searching and hand searching identified 977 articles potentially eligible for inclusion, with a final set of 16 articles selected for the review. A majority of the leadership development programs targeted preclinical students, while others spanned the entire curriculum. "Mixed settings," including both classroom and clinical and community components were common. There was a wide range of cohort sizes spanning from over 100 students to fewer than 10. Using the competencies defined by Mangrulkar et al, we determined that all of the programs described leadership skills development, including conflict management and emotional intelligence. Out of the 16 selected studies, curricula that emphasized the development of skills were evidence-based medicine and practice, and 6 curricula targeted interprofessionalism.
Conclusions:Leadership development needs to be standardized in undergraduate medical education, ideally using a competency-based framework to develop these standards. Longitudinal programs that had a didactic and project-based component received consistently high quality and effectiveness scores, as did programs with smaller cohort sizes that received more consistent mentorship and monetary investment from institutions.
Keywords: Medical education; Undergraduate; Leadership; Undergrad Medical Education (Source: MeSH-NLM).
Physicians bear immense professional responsibility: they are charged with the holistic promotion, protection, and restoration of their community’s health, as well as with the offering of guidance and consolation in the face of chronic or terminal conditions.1 Possessing effective leadership skills is essential to meeting these expectations. Leadership is defined in the U.S. Army Field Manual as “the process of influencing people by providing purpose, direction, and motivation while operating to accomplish the mission and improve the organization”.2 Leadership encompasses an array of difficult-to-master skills that must be effectively applied in clinical practice and within diverse relationships, as medicine is becoming increasingly interdisciplinary and team-based, veering away from decades of solo, autonomous practice, and driving an increase in demand for effective physician leadership.1,3–4 Too often in medical education, leadership skills are learned “accidentally,” in that it is dependent on the individual student passively observing leaders and internalizing their strategies.1,3 The Liaison Committee on Medical Education (LCME), the body responsible for overseeing the accreditation of allopathic medical schools in the United States and Canada, makes references to leadership skills in multiple competencies that MD granting schools must fulfill in order to maintain accreditation.4 The American Association of Medical Colleges (AAMC) has identified leadership as “the most critical component of success,” for future medical professionals and describes various leadership skills in the Entrustable Professional Activities, a set of proficiencies medical students are expected to be able to perform upon entering residency.5–6 Furthermore, Shaaban et al. argued in their systematic review that leadership should be the seventh competency used by the Accreditation Council for Graduate Medical Education (ACGME) to review residency programs.7 An updated systematic review of the current strategies being deployed in undergraduate medical schools is a necessary foundation to begin building new leadership education that will equip students with the tools and confidence to meet the unprecedented opportunity this season presents.8
A protocol for this systematic review was developed by drawing on the work published by Boland et Al. and the Preferred Reporting Items for Systematic Review and Meta-Analyses (PRISMA) statement.9,10 The protocol has been registered on the Prospero website, registration code CRD42021238892. International Review Board approval was not required for this study.
Comprehensive searches of literature published between 2014–2021 were conducted with databases: PubMed (MEDLINE), Embase, ERIC, PsychINFO, and Web of Sciences, using subject headings or index terms in combination with keywords including “medical students,” “undergraduate medical education,” “leadership,” “curriculum,” and “program development.” A summary of search terms for each database can be found in the Appendix. Literature search results were downloaded and imported to Covidence software, which we used to perform the title and abstract review against inclusion and exclusion criteria determined a priori (see Table 1).11 Screening of titles and abstracts was performed by ME, followed by full-text screening conducted by ME and MM in duplicate and independently. Any discrepancies in the full-text screening were resolved through discussion by the reviewers. Hand searching of references of selected articles were examined to identify any potential candidate studies for inclusion.
Table 1.Inclusion and Exclusion Criteria.
| Inclusion Criteria | Exclusion Criteria |
|---|---|
|
|
A standard form was developed for data extraction, including information about various features of the interventions such as leadership competencies and cohort sizes.12 We decided to use this framework to characterize the curricula in this review because it was developed collaboratively by educators at a variety of medical schools nationwide in an attempt to provide a consensus recommendation from diverse experiences.
This study also evaluated the effectiveness of the interventions using Kirkpatrick’s four-level hierarchy (Table 2),13 and the quality of the Interventions that formed the outcomes of the interventions outlined in the grading scale created by Hammick et al. (see Table 3).14 Extracted data was placed in a shared spreadsheet. Data extraction in each of the described areas was done independently and in duplicate by two reviewers, ME and EJ, and then compared and discussed. Any discrepancies were discussed until a unanimous decision was reached, and if a unanimous decision could not be reached, the third reviewer served as a tiebreaker.
Table 2.Inclusion and Exclusion Criteria.
| Score | Definition | No. (%) of Curricula |
|---|---|---|
| 0 | None: Outcomes not evaluated | 0 (0) |
| 1 | Reaction: Change in learners’ attitudes | 3 (18.75) |
| 2 | Learning: Modification or knowledge and/or skills | 2 (12.50) |
| 3 | Behavior: Change in behaviors as a result of learning | 6 (37.50) |
| 4 | Results: Tangible, as observed by change in the system/organizational practice; reduced cost, improved quality, efficiency, etc. | 5 (31.25) |
Quality of Evidence Using the Hammick et al Data Evaluation Model.14
| Score | Definition | No. (%) of Curricula |
|---|---|---|
| 1 | No clear conclusions can be drawn, not significant | 1 (6.25) |
| 2 | Results ambiguous, but appears to be a trend | 7 (43.75) |
| 3 | Conclusions can probably be based on the results | 6 (37.50) |
| 4 | Results are clear and very likely to be true | 2 (12.50) |
| 5 | Results are unequivocal | 0 (0) |
Comprehensive literature searching and hand searching identified 977 articles potentially eligible for inclusion in the review. The removal of 175 duplicates left 802 studies for title and abstract screening. Of 47 studies selected for full-text screening, 31 studies were excluded during full text review, and 16 (1.6%) were included in this systematic review (Figure 1). Twelve unique interventions were described, with two pairs of articles publishing different data about the same intervention at the same school.15–18
Figure 1.PRISMA Diagram of Article Selection Process.

The interventions had a mean effectiveness score of 2.6.. The mean score for quality of evidence was 2.56. Five interventions achieved the highest score for effectiveness, and none of the interventions achieved the highest score for quality of evidence. Only one study achieved the highest score for effectiveness and the next highest possible score for quality, making it the most successful intervention included in this review.26
All studies included in this review implemented interventions at LCME-accredited medical schools. A variety of settings were utilized for interventions in the included studies. Most interventions (n=13, 81.25%) included a classroom-based setting for at least part of the intervention, but only two interventions were delivered exclusively in a classroom setting. The Peak Performance educational activity at the University of North Carolina used simulation learning to enable students to take on the role of a senior resident with multiple demands on their time and resources, so that the student could practice different leadership and coping strategies. The Uniformed Services University LEAD curriculum culminates in “Operation Bushmaster,” a one-day field practicum where students are evaluated for a variety of elements including context adaptation, communication, and organizational skills.23,24
Leadership curricula were implemented at various stages within different medical schools. Interventions were most commonly offered only to preclinical students (n=7, 43.75%), followed by interventions offered only to clinical students (n=3, 18.75%), and then both groups (n=2, 12.5%). One intervention had a unique opportunity solely for MD-PhD students, and another for both clinical medical students and residents.22 Learner level was not specified for two interventions.19,21
There was a wide variation in sample size, intervention length, and curricular formats across the studies. The largest cohort size was over 200 participants in the Chicago’s UMed Program of University of Illinois College of Medicine, and the smallest was six participants in the University of Colorado’s Health Innovation Scholars Program.18,19 The average cohort size across all interventions was 53 students. Length of intervention ranged from longitudinal programs spanning all four years of the medical curriculum, such as the Quality Improvement Track implemented at the University of Chicago, to programs lasting only a summer or less than a single day, such as half-day leadership workshops offered to MD-PhD students at Vanderbilt University.20,21 There was a slight majority of stand-alone experiences (n=10, 62.5%) lasting less than 6 months as opposed to longitudinal experiences lasting multiple semesters (n=6, 37.5%).
A wide variety of leadership skills and competencies were targeted for development by the different interventions. Using the competencies defined by Mangrulkar et al., we determined that all (n=16, 100%) of the interventions promoted the development of leadership skills, including conflict management and emotional intelligence. This was closely followed by change agency (n=15, 93.75%), professionalism and ethics (n=14, 87.5%), and teamwork (n=13, 81.25%).12 Furthermore, 11 (68.75%) interventions emphasized development of skills in evidence-based medicine and practice, and six (37.5%) interventions included inter-professionalism as a competency in their program. All interventions incorporated at least two of Mangrulkar et al’s leadership competency domains into their program, which include team management, change agency, teamwork, interprofessionalism, evidence-based medicine and practice, and professionalism and ethics, and two (12.5%) of the programs incorporated all six domains.
Leadership topics were often catered to the specific objectives of each program. The Business and Leadership for Medical Students course at Boston University and the Health Innovation Scholars Program at the University of Colorado instructed students on the executive management topics and how it is affected by the healthcare policy and the supply chain’s impact on resource utilization.17,18 Project management, creating an effective meeting agenda, and adjusting to changing conditions were the focus of many interventions, such as Leaders in Innovative Care Program (LINC) at Brody School of Medicine.25 The Student Leadership Committee at Harvard Medical School provided pairs of students the opportunity to facilitate executive meetings and give presentations, followed by an opportunity to receive feedback from faculty on their performance; most survey respondents found this to be an effective approach to learn and apply principles.26 Leadership workshops conducted at Vanderbilt University solicited requests for topics from participants prior to the start of the program, and the most requested topics by students were conflict management and building a team, which became the focus of most sessions.21 The focus of the Patient-Centered Exploration in Active Reasoning, Learning and Synthesis course at the Zucker School of Medicine helped students to “think outside the box” and develop innovative approaches to running teams and solving problems through the use of complex biomedical science scenarios that students worked through in groups.15,16
The majority of studies (n=9, 56.25%) utilized a pre- and post-intervention survey to evaluate the impact on participants. A smaller proportion of studies (n=5, 31.25%) only distributed post-intervention surveys to students. The surveys sought feedback on the student’s experience with any speakers or mentors they engaged with, their opinion of the overall organization and value of the program, as well as the student’s perceptions of their own growth in various domains of leadership. Agarwal et al. specifically designed a Business and Leadership for Medical Students elective course to foster student interest in pursuing a Master in Business Administration, and the survey results noted a modest increase following the intervention, highlighting the benefit of writing questions directly related to the specific aims of the program.27 Two studies surveyed their participants both immediately and one year after the conclusion of the intervention in order to gauge the long-term impact on participants and the utility of learned skills.22,28 The Health Innovation Scholars Program (HISP) at the University of Colorado created an alumni network for all participants to join that allow them to share career developments, and consequently, many alumni have held “spread events” at their own institutions that are modeled after HISP.18 Additionally, 88% of HISP participants were involved in quality improvement in their career and 70% held leadership positions.17 Operation Bushmaster at the Uniformed Services University was unique in that intervention participants were not surveyed or interviewed to evaluate their own leadership skills and experience during the intervention.24 Instead, the participants were evaluated by superior officers before and after the intervention to assess for leadership development.24 Smithson et al. combined pre- and post-intervention surveys with reflection workbooks that participants were required to use throughout their participation in the educational activity in order to routinely evaluate their strengths and weaknesses.23 This provided robust qualitative data for program directors to improve the curriculum for future students.
The purpose of this review is to contribute to the ever-growing body of knowledge regarding best practices for leadership education in undergraduate medical education. An accurate and practical understanding of these practices is crucial to developing effective programs that will prepare medical students to be confident and effective leaders as residents and attending physicians. The 16 studies included in this review provide the basis of our recommendations.
We found that most interventions (n=11, 68.75%) achieved a score of 3 or 4 for effectiveness, reflecting changes in behavior and tangible results, respectively, and that the overwhelming majority of interventions used a mixed-method approach (n=14, 87.5%) consisting of didactic lectures, projects, seminars, simulations, among others. The interventions that achieved lower scores of 1 or 2 often lacked an opportunity for students to apply what they had learned in a didactic setting, such as the Business and Leadership course at Boston University.27 The purpose of the course was to explore nontraditional physician career paths, such as pursuing an MBA and spending most of one’s career in hospital leadership as opposed to clinical medicine. This course gave students a better understanding of the healthcare system in the United States and increased interest in pursuing leadership positions but failed to give students the chance to practice what they had learned or produce tangible results in the form of a project or presentation. The same could be said for the Physician as Leader course and the First-Year Leadership Program at the University of Michigan.28,29 The Peak Performance educational activity at the University of North Carolina utilized a simulation to give medical students the opportunity to act as senior residents with multiple demands on their time and resources so that the student could practice different leadership and coping strategies. However, when evaluating participants, it was unclear whether or not their involvement in the intervention had any specific or tangible impact on their behavior.23
The studies that achieved high scores for effectiveness described interventions that were designed for the purpose of generating a tangible result or an observable change in behavior that could be objectively assessed. We suggest using the mixed-method approach when developing leadership curricula for undergraduate medical students, to include both the benefit of supported learning and independent application of acquired skills. The ideal setup would be to begin with a didactic or instructional component that defines program goals and expectations, and follow this with an opportunity for students to work individually and in groups on a project or simulation to apply what they have learned in a meaningful way.
The interventions described in this review represent a diversity of durations and cohort sizes. There was a slight majority of stand-alone programs that lasted less than six months with respect to longitudinal programs that extended beyond six months, and within each of those categories there were programs lasting for a single half day to spanning the entire four years of the curriculum. Most programs hosted fewer than 50 students per cohort (n=12, 75%), while the other four hosted well over 100. Longitudinal programs had a higher average effectiveness score than stand-alone programs, as did programs with cohort sizes under 50 students compared to larger programs. This poses a challenge for educator, as interventions would ideally be made available to the entire student body with opportunities to engage with the program throughout the curriculum. However, a large ratio of students to faculty, financial limitations, and the packed nature of undergraduate medical curricula make it difficult for students and staff to give high-impact investment for a long period of time. Providing high impact programming for a small number of students over a short period of time is one solution, and is the strategy that was utilized by the LINC Scholars Program which received the highest scores for both quality of evidence and effectiveness in this review.25 LINC provided a group of 5 students, during an 8-week summer immersion program, with both a stipend and additional resources to fund quality improvement projects, thereby developing 15 new hospital protocols and giving students the opportunity to present their work at regional and national conferences.25 This contrasts with the University of Illinois’ UMed program, a longitudinal program spanning the entire 4-year curriculum and with more than 200 students per cohort. However, this intervention had different objectives, focusing on humanizing attitudes in its students towards marginalized community members and seeking to inspire more graduates to pursue careers in primary care, both of which were ultimately achieved.19 If the purpose of a leadership development program is to generate new, high-impact hospital or medical school policy in a short period of time, a stand-alone structure with a small group of students that can receive extensive mentoring and more substantial financial support to participants could be a promising and beneficial structure. However, if the primary goal is refining student’s leadership attitudes, developing new career interests, and creating meaningful bonds between students with common passions, a long-term program with a larger cohort might be beneficial.
Since Webb et al. published their systematic review on leadership training in undergraduate medical education, which called for improved standardization of leadership competencies and assessment strategies, very little progress has been made in this area.30 There also needs to be improved standardization in the assessment of leadership training effectiveness. Many of the programs described in this review created an in-house pre- and post-intervention survey to gauge effectiveness, and the variety between them made it difficult to assign an appropriate effectiveness score. Using a pre- and post-intervention self-assessment might have some utility for participating students, giving them a chance to reflect on strengths, weaknesses, and growth over the course of the program. Smithson et al. described an additional technique by having students complete a “reflection workbook” throughout their experience.23 The majority (14/18, 77%) of student participants completed their workbook and 91% of the students that completed their workbooks found them valuable. Some programs opted not to use surveys or self-reflection workbooks, and simply reported the number of projects completed throughout the program and a grade for their impact.17,19 During Operation Bushmaster at the Uniformed Services University, students were evaluated by faculty members for their performance, and data regarding the students’ perspective of their performance or experience was not published.24 We suggest creating a standardized rubric for faculty to evaluate students prior to and following the intervention, and basing survey questions on specific standard competencies and aims of the program.
There were several significant strengths of this review. Comprehensive literature searches were conducted by an expert searcher (medical librarian) who ensured the quality of the review.31 Furthermore, the review encapsulated a wide range of interventions in terms of geographic setting, demographics of student cohorts, and methods of delivering content that might be adaptable to a wide range of contexts.
In terms of limitations, we acknowledge that this literature review describes only published literature and articles written in English regarding leadership education in undergraduate medical education and therefore cannot account for all interventions being staged around the world. Additionally, this review only encapsulates interventions at LCME-accredited medical schools, excluding those taking place at osteopathic medical schools in the United States and medical schools around the world. It is also possible that the leadership educational domains we attempted to classify are limited or misrepresented due to the language choices or undescribed context of the study and hence, not captured in this review. Finally, this review does not include searches of all available databases; Google Scholar, Scopus and others were not included, which limits the catchment of this review.
In this article titled “Leadership Training in Undergraduate Medical Education: A Systematic Review,” the authors explore what medical schools in the United States are currently doing to develop leadership skills in their students. By understanding what is currently being done, the authors describe the practices that are most effective and might be helpful to other medical schools in creating their own curriculums for leadership development. Being an effective leader is important in medicine: physicians make decisions and manage teams in crucial settings that can be life altering for their patients, which is why it is important that leadership skills are taught early, consistently, and well. The authors reviewed multiple large databases for articles about leadership development and found 977 possible articles to include in the review. Using pre-determined inclusion and exclusion criteria, the pool was narrowed to a final set of 16 articles that were included in this review. These articles found that most medical schools begin their leadership education in the first half of a student’s medical school tenure, but very few extended the curriculum for the entirety of medical school. We also found that most medical schools used a combination of classroom-based teaching and clinical or community settings in their curriculum. Some curriculums allowed greater than 100 students to participate per class, and some had more limited cohort sizes that included 10 or fewer students to participate at a time. Furthermore, we found that different medical schools emphasized different leadership skills in their curriculums, ranging from emotional intelligence and communication to professionalism and ethics. To understand how effective these programs were at developing leadership skills and how accurate their data was, we used scoring systems from previously published articles and assigned each article a score for effectiveness and data quality. We found that the average effectiveness score for the programs was a 2.6/4, meaning that the leadership curriculums led to learning and possible changes in the behavior of learners, and the average score for quality of data was 2.56/5, which meant that the articles had some convincing data as well as some ambiguous data. When analyzing the data, we formed the following recommendations: medical schools should extend their leadership curriculums for as long as possible-ideally the entirety of medical school, the curriculum should include both didactic and practical components so that learners can have a foundation of knowledge and an opportunity to apply it in their own way, and that smaller cohort sizes with a larger amount of funding from their medical school for projects are the most effective. Finally, we found that there is no set of leadership competencies or abilities that medical schools are required to develop in their students prior to graduation. This makes it difficult for schools to be held accountable to creating effective leadership development curriculums, and to collaborate with each other. We would encourage governing bodies in the United States and around the world to world to prioritize the creation of such a standard so that schools and students can be better prepared to meet the needs of our world as physicians.
The authors would like to acknowledge the Oakland University William Beaumont School of Medicine summer internship program for providing the opportunity to begin this research.
The Authors have no funding, financial relationships or conflicts of interest to disclose.
Conceptualization, M.A.E and M.M; Methodology, M.A.E and M.M, Formal Analysis, M.A.E, E.J.J, and M.M; Investigation, M.A.E, E.J.J, and M.M; Data curation, M.A.E and M.M; Writing-Original Draft, M.A.E; Writing-Review & Editing, M.A.E, E.J.J, and M.M; Visualization, M.A.E and M.M; Supervision, M.M.
1. Schmidt JW, Linenberger SJ. Medicine: A Prescription for Medical Student Leadership Education. New Dir Stud Leadersh. 2020;2020(165):125-36.
2. Army Leadership. In: U.S. Army Field Manual. 2016;6-22. U.S. Government Printing Office.
3. Hartzell JD, Yu CE, Cohee BM, Nelson MR, Wilson RL. Moving Beyond Accidental Leadership: A Graduate Medical Education Leadership Curriculum Needs Assessment. Mil Med. 2017;182(7).
4. Standards, Publications, & Notification Forms: LCME. LCME RSS2. https://lcme.org/publications/. Accessed June 25, 2020.
5. About leadership development. AAMC. https://www.aamc.org/members/leadership/about/. Accessed June 25, 2020.
6. Core EPA Publications and Presentations. AAMC. https://www.aamc.org/what-we-do/mission-areas/medical-education/cbme/core-epas/publications. Published 2014. Accessed June 26, 2020.
7. Shaaban R, Rosenblum M, Bryson C: The seventh core competency: training residents to lead the health care team. Acad Internal Med Insight 2015;13(1): 4–5.
8. Standiford TC, Davuluri K, Trupiano N, Portney D, Gruppen L, Vinson AH. Physician leadership during the COVID-19 pandemic: an emphasis on the team, well-being and leadership reasoning. BMJ Leader. 2020;5(1):20-5.
9. Boland A, Dickinson R, Cherry MG. Doing a Systematic Review: A Student’s Guide. 2nd ed. SAGE Publications Ltd; 2017.
10. Moher D, Liberati A, Tetzlaff J, Altman DG; PRISMA Group. Preferred reporting items for systematic reviews and meta-analyses: The PRISMA statement. BMJ. 2009;339:b2535.
11. Better systematic review management. Covidence. https://www.covidence.org/. Published December 13, 2020. Accessed January 7, 2021.
12. Mangrulkar RS, Tsai A, Cox SM, et al. A Proposed Shared Vision for Leadership Development for all Medical Students: A Call from a Coalition of Diverse Medical Schools. Teach Learn Med. 2020;32(5):561-8.
13. Kirkpatrick DL. Evaluation of training. In: Craig RL, ed. Training and Development Handbook: A Guide to Human Resource Development. 2nd ed. New York, NY: McGraw-Hill; 1976.
14. Hammick M, Dornan T, Steinert Y. Conducting a best evidence systematic review. Part 1: From idea to data coding. BEME guide no. 13. Med Teach. 2010;32:3–15.
15. Ginzburg S, Deutsch S, Bellissimo J, Elkowitz D, Stern J, Lucito R. Integration of leadership training into a problem/case-based learning program for first- and second-year medical students. Adv Med Educ Pract. 2018;9:221-6.
16. Ginzburg S, Schwartz J, Gerber R et al. Assessment of medical students’ leadership traits in a problem/case-based learning program. Med Educ Online. 2018;23(1):1542923.
17. Gottenborg E, Anstett T, Diaz M, Pierce R, Sweigart J, Glasheen J. Teaching Students to Transform. Am J Med Qual. 2021;36(4):277-80.
18. Sweigart J, Tad-y D, Pierce R, Wagner E, Glasheen J. The Health Innovations Scholars Program. Am J Med Qual. 2015;31(4):293-300.
19. Girotti J, Loy G, Michel J, Henderson V. The Urban Medicine Program. Acad Med. 2015;90(12):1658-66.
20. Vinci L, Oyler J, Arora V. The Quality and Safety Track. Am J Med Qual. 2013;29(4):277-83.
21. Hsiang E, Breithaupt A, Su P, Rogers A, Milbar N, Desai S. Medical student healthcare consulting groups: A novel way to train the next generation of physician-executives. Med Teach. 2017;40(2):207-10.
22. Meador C, Parang B, Musser M, Haliyur R, Owens D, Dermody T. A workshop on leadership for senior MD–PhD students. Med Educ Online. 2016;21(1):31534.
23. Smithson S, Beck Dallaghan G, Crowner J et al. Peak Performance: A Communications-Based Leadership and Teamwork Simulation for Fourth-Year Medical Students. J Med Educ Curric Dev. 2020;7:238212052092999.
24. Barry E, Dong T, Durning S, Schreiber-Gregory D, Torre D, Grunberg N. Medical Student Leader Performance in an Applied Medical Field Practicum. Mil Med. 2019;184(11-12):653-60.
25. Lawson L, Lake D, Lazorick S, Reeder T, Garris J, Baxley E. Developing Tomorrow’s Leaders. Acad Med. 2019;94(3):358-63.
26. Rotenstein L, Perez K, Wohler D et al. Preparing health professions students to lead change. Leadersh Health Serv. 2019;32(2):182-94.
27. Agarwal A, Anderson J, Sarfaty S, Rimer E, Hirsch A. The Value of an Elective in Business and Leadership for Medical Students. J Med Pract Manage. 2015: 276-80.
28. Cadieux D, Lingard L, Kwiatkowski D, Van Deven T, Bryant M, Tithecott G. Challenges in Translation: Lessons from Using Business Pedagogy to Teach Leadership in Undergraduate Medicine. Teach Learn Med. 2016;29(2):207-15.
29. Wagenschutz H, McKean E, Mangrulkar R, Zurales K, Santen S. A first‐year leadership programme for medical students. Clin Teach. 2019;16(6):623-9.
30. Webb AM, Tsipis NE, Mcclellan TR, et al. A First Step Toward Understanding Best Practices in Leadership Training in Undergraduate Medical Education. Acad Med. 2014;89(11):1563-70.
31. Harris MR. The librarian’s roles in the systematic review process: a case study. J Med Libr Assoc. 2005;93(1):81-7.
32. Coutinho A, Bhuyan N, Gits A et al. Student and Resident Involvement in Family Medicine for America’s Health: A Step Toward Leadership Development. Fam Med. 2022;51(2):166-72.
Mallory A. Evans, 1 B.S., Fourth Year Medical Student, Oakland University William Beaumont School of Medicine, Rochester, Michigan, USA.
Eric J. James, 2 B.A., B.S., Fourth Year Medical Student, Oakland University William Beaumont School of Medicine, Rochester, Michigan, USA.
Misa Mi, 3 PhD., Professor of Foundational Medical Studies, Oakland University William Beaumont School of Medicine, Rochester, Michigan, USA.
About the Author: Mallory Evans is a fourth-year medical student at Oakland University William Beaumont School of Medicine in Rochester, Michigan. Eric James is a fourth-year medical student and Oakland University William Beaumont School of Medicine in Rochester, Michigan. Dr. Misa Mi is a professor in Foundational Medical Studies at Oakland University William Beaumont School of Medicine in Rochester, Michigan.
Correspondence: Mallory A. Evans. Address: 586 Pioneer Dr, Rochester, MI 48309, United States. Email: mhoevet@oakland.edu
Editor: Francisco J. Bonilla-Escobar Student Editors: Yusuff Adebisi & Patricio García-Espinosa Copyeditor: Michael V. Tavolieri Proofreader: Laeeqa Manji Layout Editor: Ana Maria Morales Process: Peer-reviewed
Supplementary Material AppendixSearch Strategies
| Database | Platform | Search Strategies |
|---|---|---|
| PubMed | NLM | students, medical [mh] OR schools, medical [mh] OR education, medical, undergraduate [mh] OR “medical student” [ti] OR “medical students” [ti] OR “medical school” [ti] OR “medical schools” [ti] OR “undergraduate medical education” [ti]) AND (leadership [mh] OR leadership[ti]) AND (education [mh] OR learning [mh] OR program development [mh] OR program Evaluation [mh] OR curricul* OR course*[ti] OR program* [ti] OR educate* [ti] OR learn*[ti] OR teach*[ti] OR instruct*[ti]) |
| Embase | ELSEVIER | ('medical school'/exp OR ‘medical students’/exp OR ‘undergraduate medical education’/exp) AND ‘leadership’/exp/mj AND ('education'/exp OR ‘learning’/exp) OR ('medical student' OR ‘medical students’ OR ‘medical school’ OR ‘medical schools’ OR ‘undergraduate medical education’) AND leadership AND ('program development' OR ‘program evaluation’ OR curricul* OR course* OR program* OR educat* OR learn* OR teach* OR instruct*) |
| ERIC | ProQuest | (MAINSUBJECT.EXACT(“medical schools” OR “medical students”) OR “medical student” OR “medical students” OR “medical school” OR “medical schools” OR “undergraduate medical education") AND (MAINSUBJECT.EXACT(“Leadership”) OR leadership) AND (MAINSUBJECT.EXACT(“program evaluation” OR “program development” OR “curriculum” OR “courses” OR “learning” OR “instructional development” OR “instructional design” OR “instructional development") OR “Program Development” OR “Program Evaluation” OR curricul* OR course* OR program* OR learn* OR teach* OR instruct*) |
| PsychINFO | ProQuest | (“medical student” OR “medical students” OR “medical school” OR “medical schools” OR “undergraduate medical education”) AND leadership AND (“Program Development” OR “Program Evaluation” OR curricul* OR course* OR program* OR learn* OR teach* OR instruct*) |
| Web of Sciences | Clarivate | (“medical student” OR “medical students” OR “medical school” OR “medical schools” OR “undergraduate medical education”) AND leadership AND (“Program Development” OR “Program Evaluation” OR curricul* OR course* OR program* OR learn* OR teach* OR instruct*) |
Summary of Systematic Review Findings
| First Author, Date | Length of Intervention, Number of Students per Cohort | Learner Level (number of students) | Curricular Format | Educational Setting | Curricular Domains based on Mangrulkar et al # | Quality of Evidence Score using Hammick et al | Effectiveness Score using Kirkpatrick's 4-level Hierarchy |
|---|---|---|---|---|---|---|---|
| Agarwal 201527 | 2 years, 22 | Preclinical | Stand-Alone | Mixed (didactic, case-based) | A, B, D, F | 2 | 2 |
| Barry 201824 | 1 day, >100 | Clinical | Stand-Alone | Field practicum | A, B, C, F | 2 | 3 |
| Cadieux 201728 | 1 week, 172 | Preclinical | Stand-Alone | Mixed (didactic, TBLs, small group discussion) | A, B, C, D, F | 2 | 1 |
| Coutinho 201932 | 1 year, 36 | Other (Clinical and Residents) | Stand-Alone | Mixed (projects, online, workshops) | A, E | 2 | 4 |
| Ginzburg 2018*15 | 2 years, 44 | Preclinical | Longitudinal | Mixed (PBL, CBL, workshop) | A, B, C, E, F | 4 | 3 |
| Ginzburg 2018*16 | 2 years, 44 | Preclinical | Longitudinal | Mixed (PBL, CBL, workshop) | A, B, C, E, F | 3 | 3 |
| Girotti 201519 | 4 years, >200 | Preclinical and Clinical | Longitudinal | Mixed (seminar, online, project) | A, B, C, E, F | 3 | 4 |
| Gottenborg 2020**17 | 5 weeks, <10 | Preclinical | Stand-Alone | Mixed (didactic, project, workshop) | A, B, C, D, E, F | 3 | 4 |
| Hsiang 201821 | 6 months, 23 | Not described | Longitudinal | Mixed (didactic, workshop, project) | A, B, C, E, F | 2 | 4 |
| Lawson 201925 | 8 weeks, 5 | Clinical | Stand-Alone | Mixed (project, workshop) | A, B, C, D, E, F | 4 | 4 |
| Meador 201622 | 1 day, 23 | Clinical (M4 MD-PhD students) | Stand-Alone | Mixed (didactic, workshop) | A, B, C, F | 3 | 3 |
| Rotenstein 201926 | 1 year, 33 | Not described | Longitudinal | Mixed (didactic, project) | A, B, C, D, E, F | 2 | 3 |
| Smithson, 202023 | 4 weeks, 18 | Clinical | Stand-Alone | Simulation | A, B, C, D, E, F | 2 | 1 |
| Sweigart 2016**18 | 5 weeks, 6 | Preclinical | Stand-Alone | Mixed (seminar, workshop, project) | A, B, C, E, F | 3 | 3 |
| Vinci 201420 | 4 years, 23 | Preclinical and Clinical | Longitudinal | Mixed (project, workshop) | A, B, E | 3 | 2 |
| Wagenschultz 201929 | 1 year, 166 | Preclinical | Stand-Alone | Didactic | A, B, C, F | 1 | 1 |
Cite as Evans MA, James EJ, Mi M. Leadership Training in Undergraduate Medical Education: A Systematic Review. Int J Med Stud. 2023 Jan-Mar;11(1):58-66.
Copyright © 2023 Mallory A. Evans, Eric J. James, Misa Mi
This work is licensed under a Creative Commons Attribution 4.0 International License.
International Journal of Medical Students, VOLUME 11, NUMBER 1, March 2023