Editorial
Writing Case Reports: Teaching and Tuition Techniques, and the Improvement of Clinical
Diagnostic Reasoning
Yosuke Kakisaka12, Mayu Fujikawa1, Schuyler Gaillard3
doi: http://dx.doi.org/10.5195/ijms.2016.157
Volume 4, Number 3: 88-90
The case report is a time-honored, important, integral, and widely accepted component
of the medical literature.1 Reporting of cases illustrating new or rare clinical phenomena is highly encouraged
to extend medical knowledge through patient treatment. The process of writing a case
report is essential to medicine and patient care, as described by Osler.2
Writing Case Reports Enhances Clinical Diagnostic Reasoning
We present two example cases which illustrate how writing case reports enhances clinical
diagnostic reasoning. The first important case report of author YK described a patient
encountered during a pediatric residency over 10 years ago. A 13-year-old girl visited
a pediatric outpatient clinic. Her complaint was periodic periumbilical abdominal
pain with episodes lasting several hours. This symptom was stereotypical between episodes
and remitted spontaneously every time. However, routine medical examination was unremarkable.
The process of exploring the pathophysiology of an abdominal pain through literature
search was tremendously intriguing. Several case reports indicated abdominal pain
as one of the various extra-cephalic symptoms of migraine. The patient was finally
diagnosed with abdominal migraine, a migraine variant, and her abdominal pain was
relieved with sumatriptan administration. This case was published in the Japanese
literature.3 This experience was the departure point of YK’s exploration of the curious pathophysiology
of migraine and its variants. Since then, this rare extracephalic symptom has been
added to the list of screening symptoms for patients complaining of headaches during
history taking.
YK subsequently encountered the case of a 34-year-old female with a family history
of migraines. She was referred to our clinic for evaluation of recurrent epigastric
pain with severe cramping, which had started at age 9 years with a frequency of once
per month. Gastrointestinal evaluation was performed between attacks and found no
abnormality. The patient also complained of severe throbbing headaches lateralized
to the right temporal region, which appeared at age 24 years. These headaches lasted
for a maximum of several days per episode, with a frequency of once per month. The
patient had a prior diagnosis of temporal lobe epilepsy at a previous hospital based
on electroencephalography indicating temporal intermittent rhythmic delta activity
in the left hemisphere without obvious spikes. However, YK’s initial assessment suspected
abdominal migraine because of her abdominal symptoms and long duration of intense
pain. In contrast, mesial temporal lobe epilepsy typically presents with short epigastric
discomfort. The coexistence of cephalic migraines also supported the diagnosis of
abdominal migraine. Further investigation of her epigastric attacks revealed the presence
of photophobia and phonophobia during her abdominal pain episodes. Consequently, she
was diagnosed with abdominal migraine. Sumatriptan administration successfully controlled
the abdominal pain episodes.4 Previous experience of researching and summarizing knowledge of abdominal migraine,
undertaken for the aforementioned case report,3 facilitated the correct diagnosis.
Clinical diagnostic reasoning is defined as “the thinking process to reach the appropriate
conclusions for diagnosis and treatment.”5 Clinical diagnostic reasoning is based on fundamental factors: knowledge about disease,
context of patient’s history, and clinical experience.5 All of these aspects are essential in case writing. Figure 1 describes a theoretical model of the relationship between clinical diagnostic reasoning
and case writing. The first step of clinical diagnostic reasoning is acquiring clinical
information based on the patient’s history (shaded box in Figure 1). The second step is to understand the represented problem, which is the process
of formulating a hypothesis. To reach the most appropriate diagnosis from the hypothesis,
search for the defining and discriminating features of each possible disease under
consideration with additional targeted data gathering and literature search.5
Figure 1.
Proposed Modification of Bowen’s Model of Key Elements of Clinical Diagnostic Reasoning5
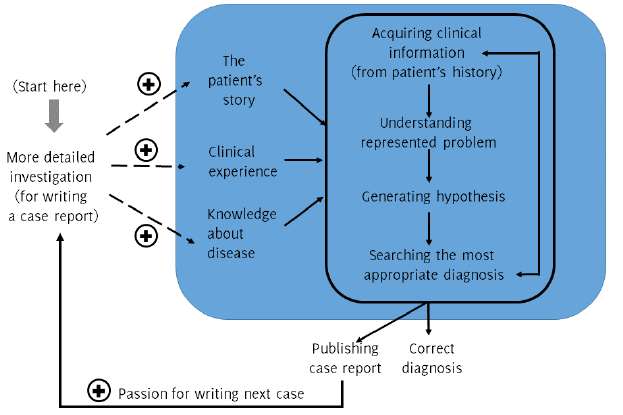
Dashed arrows indicate the potential effects of writing and publishing case reports
about disease X on clinical diagnostic reasoning applied to subsequent cases of disease
X.
The process of case writing necessitates thorough investigation of the context of
patient history, in addition to increasing clinical experience by reviewing clinical
and imaging data. Furthermore, case writing requires analysis of the literature that
describes similar symptoms. Both clinical interactions and literature review increase
specific disease knowledge. Therefore, case writing provides the opportunity to combine
knowledge about disease, the context of the patient history, and clinical experience.
Therefore, we consider that publishing case reports (about disease X) enhances the
physician’s clinical diagnostic reasoning skills (about disease X), which will be
helpful in following further cases (of disease X). In the following section, we introduce
the theoretical process of case writing and how it may benefit clinical diagnostic
reasoning.
Writing Case Reports as Medical Education
We recently launched an educational case writing program for medical students at Tohoku
University School of Medicine. The program consists of two parts: (1) a didactic lecture
for learning the principles of case writing, and (2) a hands-on case writing practice
to apply the learned skills in a clinical case. The didactic lecture focuses on identifying
the topic for a case report. A desirable topic should include both scientific significance
and novel knowledge illustrated by the report. The topic may describe the patient’s
symptoms (e.g. clinical course, imaging), utility of a medical modality, or even specific
clinical actions (e.g. hints for efficacious history taking). We recommend three steps
to identify the topic for a case report: (1) to read related case reports in order
to increase knowledge of the patient’s condition; (2) to make a table to compare the
current patient’s symptoms with previously described symptoms; and (3) to critically
assess whether the topic has reportable significance as a case report. The details
and educational efficacy of the didactic part of this program are presented separately
in a Letter to the Editor published in this issue of International Journal of Medical Students (IJMS).6
Students in the program write case reports under the supervision of faculty staff
in the second part of the program. Figure 2 illustrates the developmental course of writing skill through the program. After
the lecture on the principles of case writing, the students begin writing actual case
reports. Initial drafts produced by the students typically need drastic correction.
Brainstorming or Socratic questioning is often effective in enhancing students critical
thinking, through questions such as “what is the main topic of this case?”, “how can
we describe it scientifically?”, and “how should we form a hypothesis of the mechanism
under discussion?” Multiple discussion sessions between students and faculty increase
the quality of the manuscript, which in turn improves case writing skills and the
level of theoretical understanding about the case writing principles. Each subsequent
draft should require less guidance from the faculty, and the students will eventually
achieve a satisfactory skill level (n-th paper of Figure 2).
Figure 2.
Feedback in the Process of Improving Skills
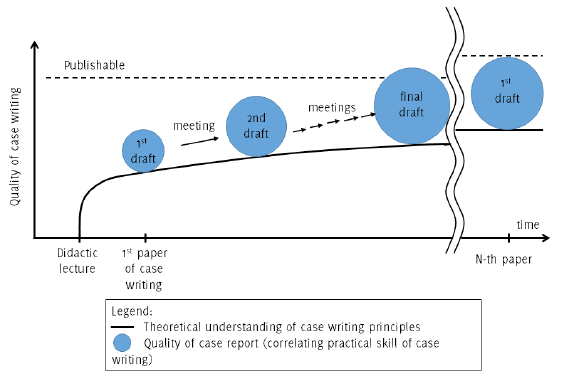
After the didactic lecture (step 1) about the principles of case writing, students
begin the process of actual case writing. Initially, drafts are immature even after
receiving the lecture, as both theoretical understanding and practical skills of case
writing lack experience. Multiple meetings between the student and advisor increase
the quality of the current case report, which correlates with the practical skills
of case writing, as well as increase the theoretical understanding of case writing
principles. Therefore, the quality of the first draft of the n-th paper will be higher
than that of the first paper.
Medical students often struggle to reach the correct diagnosis based on clinical diagnostic
reasoning because they often lack the three skill factors (knowledge of disease, context
of patient’s history, and clinical experience). We believe that multiple experiences
with writing case reports will help improve the knowledge of clinical diagnostic reasoning
among medical students. In particular, once a medical student publishes a case report,
the sense of accomplishment will bring pleasure and reward for the finished case report
and motivate the student to undertake the task of writing another case report.7
In the future, the educational case writing program may allow wider opportunities
to include medical students in distant or rural areas with limited opportunity for
writing scientific papers. Using a high-definition telemedicine system, students interested
in learning about case report writing can access our program with face-to-face tuition.
To promote this program to students in remote areas, we have started to provide lectures
and discussion via the telemedicine system. Integration of such new teaching techniques
and developed technologies may establish a new approach to medical education.
Acknowledgments
We would like to thank Francisco Javier Bonilla-Escobar, Editor-in-Chief of IJMS,
for the invitation to write an Editorial to the Journal regarding our experience on
writing case reports.
Conflict of Interest Statement & Funding
The authors have no funding, financial relationships, or conflicts of interest to
disclose.
Author Contributions
Conceptualization: YK. Writing, Critical revision of the manuscript, Approval of the
final version: YK, MF, SG.
References
1. Ortega-Loubon C, Correa-Marquez R. Writing a case report: a work of art. Int J Med Students. 2014 Jul-Oct;2(3):90–1.
2. Thayer WS. Osler, the teacher. In: Sir William Osler, Bart. Baltimore: Johns Hopkins Press; 1920. p. 51–2.
3. Kakisaka Y, Matsuki S, Miura Y, Nakayama S, Sato T, Tanabu M, et al. [Successful treatment with sumatriptan in a case with abdominal migraine]. Japanese J Clin Pediatr. 2004 Nov;57(11):2285–9. Japanese
4. Kakisaka Y, Jin K, Kato K, Iwasaki M, Nakasato N. Temporal intermittent rhythmic delta activity and abdominal migraine. Neurol Sci. 2014 Apr;35(4):627–8.
5. Bowen JL. Educational strategies to promote clinical diagnostic reasoning. N Engl J Med. 2006 Nov 23;355(21):2117–25.
6. Kakisaka Y. Structured didactic education program for writing case reports can motivate medical
students. Int J Med Students. 2016 Sep-Dec;4(3): Forthcoming.
7. Petrusa ER, Weiss GB. Writing case reports: an educationally valuable experience for house officers. J Med Educ. 1982 May;57(5):415–7.
Yosuke Kakisaka, 1 Department of Epileptology, Tohoku University Graduate School of Medicine, Sendai,
Miyagi, Japan.
2 Department of Pediatrics, Tohoku University Graduate School of Medicine, Sendai, Miyagi, Japan.
Mayu Fujikawa, 1 Department of Epileptology, Tohoku University Graduate School of Medicine, Sendai,
Miyagi, Japan.
Schuyler Gaillard, 3 Department of Brain and Cognitive Sciences, Massachusetts Institute of Technology,
Cambridge, MA, USA.
About the Author: Yosuke Kakisaka is a pediatrician and epileptologist at Tohoku University Graduate
School of Medicine in Sendai, Japan.
Correspondence Yosuke Kakisaka. Address: Department of Epileptology, Tohoku University Graduate
School of Medicine, 2-1 Seiryo-machi, Aoba-ku, Sendai, Miyagi 980-8575, Japan. Email:
kakisuke@mui.biglobe.ne.jp
Cite as: Kakisaka Y, Fujikawa M, Gaillard S. Writing case reports: teaching and tuition techniques, and the improvement of clinical diagnostic reasoning. Int J Med Students. 2016 Sep-Dec;4(3):88-90.
Copyright © 2016 Yosuke Kakisaka, Mayu Fujikawa, Schuyler Gaillard.
International Journal of Medical Students, VOLUME 4, NUMBER 3, December 2016

