Case Report
Pneumatocele-Induced Pneumothorax in a Patient with Post-COVID-19 Pneumonitis. A Case
Report
Kevin O. Wortman1, Kevin O. Wortman2
doi: http://dx.doi.org/10.5195/ijms.2021.1012
Volume 9, Number 3: 223-226
Received 19 04 2021:
Rev-request 01 05 2021:
Rev-request 30 07 2021:
Rev-recd 07 05 2021:
Rev-recd 07 08 2021:
Accepted 11 08 2021:
Publication 24 08 2021
ABSTRACT
Abstract
Background:
The COVID-19 pandemic has been challenging medical professionals and facilities for
over a year now. Much of the literature describes pathologic lung changes and complications
associated with SARS-CoV-2, with pneumothorax and pneumatoceles not being uncommon.
The Case:
We describe a case involving a patient that presented to the emergency department
with a pneumothorax. Three weeks prior, the patient was hospitalized for 10 days in
acute respiratory distress secondary to SARS-CoV-2 pneumonia, which did not require
ventilator support. Follow up imaging revealed a 7 cm (AP) × 4.6 cm (transverse) ×
2.5 (cc) cm pneumatocele.
Conclusion:
We speculate that antecedent rupture of an unrecognized pneumatocele likely caused
lung collapse leading to the patient's pneumothorax. This review delves into the etiology
of both pneumothoraxes and pneumatoceles along with their relation to SARS-CoV-2 pneumonia.
Keywords:
COVID-19;
Pneumatocele;
Pneumothorax;
Tension Pneumothorax;
SARS-CoV-2 (Source: MeSH-NLM).
Introduction
This article describes the clinical course of a patient that presented to an Emergency
Department (ED) with a spontaneous pneumothorax post-SARS-CoV-2 pneumonia, with a
pneumatocele discovered on radiography. While pneumatoceles are more common within
the post-pneumonia, pediatric population,1 a retrospective study has shown pneumatocele development as a missed diagnosis in
up to 37% of their 78 patients with the coronavirus disease.2 Additional studies show varying numbers with pneumatocele development seen in 10%
of 81 symptomatic patients in the study by Shi et al.3 and in 5.3% of 57 SARSCoV-2 positive patients in the study Qi et al.4 Radiologic studies use terms such as ‘cystic air spaces,’2 ‘cystic changes,’3 and ‘emphysema,’4 which are synonymous with pneumatocele. Pneumatoceles, in relation to COVID-19, are
highly variable in size; some are categorized as ‘giant bullae’5 and typically present in multiples rather than a singular lesion.6
A predictable complication of pneumatoceles is pneumothorax.1,5 A few case studies report pneumothoraxes as a rare complication of COVID-19.7,8 Risk factors for pneumothorax include young age, chest trauma,1 individuals with imaging demonstrating fibrotic lung changes,9 individuals with a more severe clinical course, prolonged pneumonitis duration, and
higher neutrophil counts.10 In our experience with COVID-19 management, pneumothorax is more common in mechanically
ventilated patients, which is as high as 13% in one study,11 likely due to barotrauma. However, patients are presenting with pneumothoraxes well
before ventilatory support is provided.
The Case
A 28-year-old African American male presented to an ED reporting chest and back pressure/pain
along with shortness of breath. Three weeks prior, the patient presented to the same
ED in respiratory distress secondary to PCR confirmed SARS-CoV-2 pneumonia. He was
hospitalized for 10 days and received oxygen, remdesivir, dexamethasone, tocilizumab,
and enoxaparin therapy. The patient did not require mechanical ventilation during
his prior hospitalization.
Highlights:
- COVID-19 recovery complications are not emphasized in literature as much as pathophysiology,
clinical treatment, and epidemiology.
- As the pandemic is taking its course, many patients are recovering from COVID-19 but
may be at risk for complications.
- To ensure pneumatoceles are diagnosed and tracked in anticipation of spontaneous pneumothorax,
we recommend that patients post-COVID-19 pneumonitis are assessed radiographically
before hospital discharge and within two weeks after discharge. This will lead to
early detection of pneumatoceles and will provide an insight into a subgroup of COVID-19
patients that may be at risk for multiple pathological pulmonary events after COVID-19
hospitalization. This will aid physicians in being cognizant regarding this subgroup
of patients who will benefit from a more stringent monitoring.
- Larger studies are warranted to distinguish between Long COVID/Long-haul COVID/Post-acute
sequelae SARS-CoV-2 (PASC) and Post-COVID-19 pneumonitis as well as the complications
related to both these conditions.
During the current presentation to the ED for respiratory distress the patient was
saturating at 82% on room air, which improved to 92% on 4 liters per minute of nasal
cannula oxygen. Chest radiographs revealed a large right pneumothorax with subsequent
mediastinal shift to the left (Figure 1). A pigtail catheter was inserted at the 2nd intercostal space along the midclavicular line.
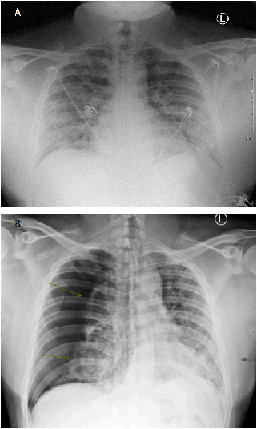
Figure 1.
(A): Patient's chest x-ray taken during the previous hospitalization, showing extensive
bilateral interstitial airspace opacities throughout the right and left lungs. (B):
Patient's chest x-ray at presentation showing a large right pneumothorax, with the
majority of the right lung collapsed. There is mild to moderate mediastinal shift
to the left. Both lungs show evidence of bilateral airspace/interstitial disease.
After two days, the catheter accidentally dislodged from the patient's pleural space
and serial CXRs were performed to determine whether the pneumothorax had resolved.
Although the patient was clinically asymptomatic, the radiographs showed worsening
of the pneumothorax; therefore, a pigtail catheter was reinserted at the 4th intercostal space along the mid axillary line. The CXR on Day 4 also showed formation
of a round lesion with central air-fluid levels that was speculated to be a pneumatocele
(Figure 2). On subsequent imaging, the pneumothorax appears to have improved, although not
completely resolved (Figure 3). The lesion was monitored by a local pulmonologist and treated daily with fluticasone
inhaled therapy, until resolution 7 weeks later.
Figure 2.
Follow up chest x-ray on Day 4 showing an unresolved right pneumothorax (20-30%) and
ill-defined pulmonary opacities throughout both lungs, deduced to be bilateral interstitial
disease. A round lesion with central air-fluid levels formed within the right mid
lung and was speculated to be a pneumatocele
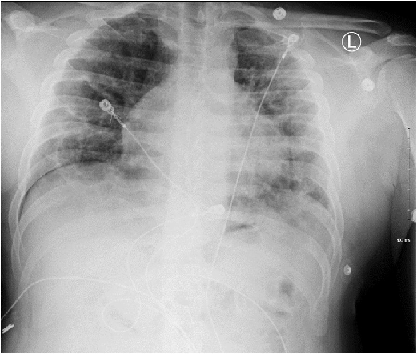
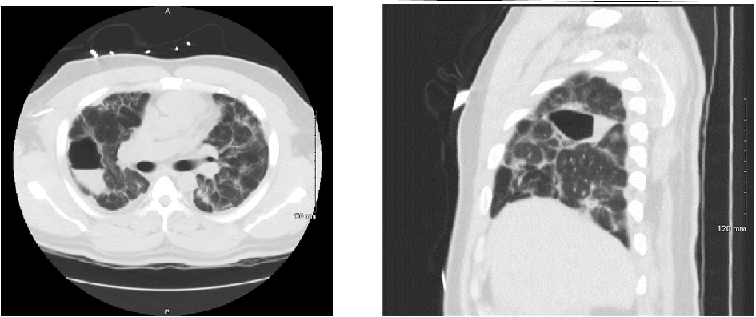
Figure 3.
Non-contrast CT scans showing resolution of the pneumothorax. Laterally in right upper
lobe, there is oval-shaped lucent lesion measuring 7 cm (AP) × 4.6 cm (transverse)
× 2.5 cm (cc). Wall is thin and barely perceptible. Inner margin of the cavity is
smooth. There is an internal air-fluid level. It is difficult to tell if this collection
is tracking along the minor fissure. Numerous scattered ground-glass pulmonary opacities
are present throughout each lung.
Discussion
Textbook pneumothorax patients often have a history of a connective tissue disorder,
such as Marfan syndrome or Ehlers-Danlos syndrome, and/or have a characteristic marfanoid
habitus, COPD, smoking, or pregnancy.12 Our patient denied a recent history of trauma, denied a history of smoking, and had
a body mass index of 35.9 kg/m2. This patient does not fit into the standard demographic of patients at an increased
risk of pneumothorax and there are still uncertainties regarding COVID-19-related
lung changes and complications. This led us to hypothesize that pneumatoceles may
well be a potential mechanism behind this pneumothorax.
The percentage of COVID-19 cases that are complicated by pneumatocele development
has yet to be determined. Pneumatoceles typically appear 5-6 days after the infectious
process secondary to SARS-CoV-2.13 However, spontaneous pneumothorax is a known, rare complication of COVID-19 and can
occur in the absence of mechanical ventilation,14 with studies showing that pneumothorax occurs within a window of 14–37 days after
hospitalization.7 Pneumothorax is also not a common sequel to pneumatoceles as the majority of pneumatoceles
resolve spontaneously within a few weeks to a year, without intervention.1 In this case, while no pneumatocele was identified before or at presentation, antecedent
rupture of an unacknowledged pneumatocele could have led to the pneumothorax. The
single pneumatocele lesion likely formed due to parenchymal inflammation secondary
to acute respiratory distress syndrome (ARDS), which is not uncommon.15 There have not been any studies that deduce a specific mechanism for COVID-19 infection
itself eliciting pneumatocele formation, without pneumonitis underplay.
Pneumothoraxes are rarely fatal; however, they have recurrence rate of up to 32% within
12 months according to one meta-analysis.16 This patient's pneumothorax pathology could have occurred either through pneumatocele
rupture, which has been reported in other case studies,8 or due to COVID-19-induced pulmonary parenchymal injury and necrosis with development
of air leaks into the pleural cavity. While the former has not been thoroughly studied
due to the relative novelty of COVID-19, the latter was noted previously during the
SARS outbreak.16,17 If pulmonary necrosis led to pneumothorax, then the pneumatocele seen in this patient
was likely an incidental finding.
As per the World Health Organization (WHO), most COVID-19 patients experience a mild-to-moderate
clinical course, with 10-15% of patients progressing to a severe clinical presentation
and 5% progressing to critical illness. In general, recovery can take anywhere from
2–6 weeks, depending on the severity of the case. Unfortunately, some patients experience
symptoms for weeks to months, regardless of disease severity.18 These patients were colloquially deemed ‘long COVID’ or ‘COVID long-haulers,’ which
later became ‘post-acute sequelae of SARSCoV-2 (PASC)’. Studies suggest that roughly
one-third of those infected with SARS-CoV-2, whether asymptomatic during infection
or not, may develop PASC.19,20 According to a study conducted by Lambert et al.21, of the 5,875 COVID-19 survivors surveyed, 5,163 reported symptoms persisting longer
than 21 days. The most common symptom reported was fatigue (79.0%) and followed by
headache/migraines (55.3%), shortness of breath (55.3%), difficulty concentrating
(53.6%), cough (49.0%), changed sense of taste (44.9%), diarrhea (43.9%), muscle/body
aches (43.5%), and heart palpitations (39.5%).21 Another study surveying 3,762 respondents from 56 countries reported the most frequent
symptoms being fatigue (77.7%), post-exertional malaise (72.2%), and cognitive dysfunction
(55.4%).22 Risk factors for PASC include hypertension, obesity, prior mental health conditions,21 and female gender (two times increased risk as compared to males).23 While COVID-19 is at the forefront of research, a clear distinction must be made
between individuals suffering from PASC and post-COVID-19 pneumonitis, as well as
their respective complications. Larger retrospective cohort studies and case reports,
pertaining to both PASC and Post-COVID-19 pneumonitis, are warranted.
Conclusion
Cystic lesions, pneumatoceles, and subsequently pneumothoraxes are likely to result
from prolonged SARS-CoV-2 pneumonia causing air leaks. This is similar to the clinical
course observed in patients with SARS, caused by a virus within the same Coronaviridae
family, during the 2003 outbreak. To ensure pneumatoceles are diagnosed and tracked
in anticipation of spontaneous pneumothorax, we recommend that patients with post-COVID-19
pneumonitis, especially those given ventilator support, are assessed radiographically
before hospital discharge and within two weeks after discharge. This will lead to
early detection of pneumatoceles and will provide an insight into a sub-group of COVID-19
patients that may be at risk for multiple pathological pulmonary events after COVID-19
hospitalization. This could physicians in being cognizant regarding this sub-group
of patients, who could benefit from more stringent monitoring. Furthermore, larger
studies are warranted to distinguish between Long COVID/Long-haul COVID/Post-acute
sequelae SARS-CoV-2 (PASC) and Post-COVID-19 pneumonitis, as well as the complications
related to both these conditions.
Acknowledgments
None.
Conflict of Interest Statement & Funding
The Authors have no funding, financial relationships or conflicts of interest to disclose.
Author Contributions
Conceptualization, Investigation, Resources: KOW II & KOW Sr. Data Curation, Project
Administration, Supervision, Writing – Original Draft Preparation: KOW II. Writing
– Review & Editing: KOW Sr.
References
1. Jamil A, Kasi A. Pneumatocele. StatPearls. Treasure Island (FL): StatPearls Publishing. 2021 Jan. Available from: https://www.ncbi.nlm.nih.gov/books/NBK556146/. Last updated Aug 11, 2021; cited Apr 10, 2021.
2. Werberich GM, Marchiori E, Barreto MM, Rodrigues RS. Computed Tomography Findings in a Brazilian Cohort of 48 Patients with Pneumonia due
to Coronavirus Disease. Rev Soc Bras de Med Trop. 2020 Jul 20;53:e20200405.
3. Shi H, Han X, Jiang N, Cao Y, Alwalid O, Gu J, et al. Radiological Findings from 81 Patients with COVID-19 Pneumonia in Wuhan, China: a
Descriptive Study. Lancet Infect Dis. 2020 Apr;20(4):425–34.
4. Qi S, Guo H, Shao H, Lan S, He Y, Tiheiran M, et al. Computed Tomography Findings and Short-Term Follow-up with Novel Coronavirus Pneumonia. MedRxiv 2020:20042614 [Preprint].
5. Sun R, Liu H, Wang X. Mediastinal Emphysema, Giant Bulla, and Pneumothorax Developed during the Course of
COVID-19 Pneumonia. Korean J Radiol. 2020 May;21(5):541–4.
6. Reed JC. Multiple Lucent Lesions. In: Chest Radiology: Plain Film Patterns and Differential Diagnoses. 7th ed. Elsevier. 2017.
7. Chen N, Zhou M, Dong X, Qu J, Gong F, Han Y, et al. Epidemiological and Clinical Characteristics of 99 Cases of 2019 Novel Coronavirus
Pneumonia in Wuhan, China: a Descriptive Study. Lancet. 2020 Feb 15;395(10223):507–13.
8. Mallick T, Dinesh A, Engdahl R, Sabado M. COVID-19 Complicated by Spontaneous Pneumothorax. Cureus. 2020 Jul 9;12(7):e9104.
9. Zantah M, Castillo ED, Townsend R, Dikengil F, Criner GJ. Pneumothorax in COVID-19 Disease-Incidence and Clinical Characteristics. Respir Res. 2020 Sep 16;21:236.
10. Sihoe ADL, Wong RHL, Lee ATH, Lau LS, Leung NYY, Law KI, et al. Severe Acute Respiratory Syndrome Complicated by Spontaneous Pneumothorax. Chest. 2004 Jun;125(6):2345–51.
11. Chopra A, Al-Tarbsheh AH, Shah NJ, Yaqoob H, Hu K, Feustel PJ, et al. Pneumothorax in Critically Ill Patients with COVID-19 Infection: Incidence, Clinical
Characteristics and Outcomes in a Case Control Multicenter Study. Respir Med. 2021 Aug 1;184:106464.
12. McKnight CL, Burns B. Pneumothorax. StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing. 2021 Jan. Available from: https://www.ncbi.nlm.nih.gov/books/NBK441885/. Updated Aug 11, 2021; cited Apr 10, 2021.
13. Sanivarapu, RR, Farraj K, Sayedy N, Anjum F. Rapidly Developing Large Pneumatocele and Spontaneous Pneumothorax in SARS-CoV-2 Infection. Respir Med Case Rep. 2020 Dec 2;31:101303.
14. Zantah M, Castillo ED, Townsend R, Dikengil F, Criner GJ. Pneumothorax in COVID-19 Disease-Incidence and Clinical Characteristics. Respir Res. 2020 Sep 16;21:236.
15. Chennu G, Przydzial P, Tchao Y, Isedeh A, Madan N. Pneumatocele after Acute Respiratory Distress Syndrome in an Adult Patient: A Case
Report. Case Rep Acute Med. 2020 Oct 30;3(3):73–8.
16. Walker SP, Bibby AC, Halford P, Stadon L, White P, Maskell NA. Recurrence Rates in Primary Spontaneous Pneumothorax: a Systematic Review and Meta-Analysis. Eur Respir J. 2018 Sep 6;52(3):1800864.
17. Kao HK, Wang JH, Sung CS, Huang YC, Lien TC. Pneumothorax and Mortality in the Mechanically Ventilated SARS Patients: a Prospective
Clinical Study. Crit Care. 2005 Jun 22;9:R440.
18. World Health Organization. Coronavirus Update 36 What We Know About Long-Term Effects of COVID-19: The Latest
on the COVID-19 Global Situation & Long-Term Sequelae. Available from: https://www.who.int/publications/m/item/update-36-long-term-effects-ofcovid-19. Updated September 9, 2020; cited August 24, 2021.
19. Nehme M, Braillard O, Alcoba G, Perone SA, Courvoisier D, Chappuis F, et al; COVIDCARE Team. COVID-19 Symptoms: Longitudinal Evolution and Persistence in Outpatient Settings. Ann Intern Med. 2021 May;174(5):723–5.
20. Huang Y, Pinto MD, Borelli JL, Mehrabadi MA, Abrihim H, Dutt N, et al. COVID Symptoms, Symptom Clusters, and Predictors for Becoming a Long-Hauler: Looking
for Clarity in the Haze of the Pandemic. MedRxiv 2021:21252086 [Preprint].
21. Lambert N, El-Azab SA, Ramrakhiani NS, Barisano A, Yu L, Taylor K, et al; Survivor Corps. COVID-19 Survivors’ Reports of the Timing, Duration, and Health Impacts of Post-Acute
Sequelae of SARS-CoV-2 (PASC) Infection. MedRxiv 2021:21254026 [Preprint].
22. Davis HE, Assaf GS, McCorkell L, Wei H, Low RJ, Re’em Y, et al. Characterizing Long COVID in an International Cohort: 7 Months of Symptoms and Their
Impact. MedRxiv 2020:20248802 [Preprint].
23. Nabavi N. Long Covid: How to Define It and How to Manage It. Brit Med J. 2020 Sep 7;370:m3489.
Kevin O. Wortman, 1 M.S., Edward via College of Medicine, Auburn, Alabama, United States
Kevin O. Wortman, 2 R.N. BSN CCRN.
About the Author: Kevin Wortman II is currently a 4th year osteopathic medical student of Edward via
COM- Auburn, AL USA; which is a 4-year program. He is also the recipient of the 2019
Sherry Arnstein Minority Student scholarship, funded by the American Association of
Colleges of Osteopathic Medicine, and 2020 J. W. Darden scholarship, funded by the
J. W. Darden Foundation.
Correspondence: Kevin O. Wortman II. Address: 910 S Donahue Dr, Auburn, AL 36832, United States.
Email: Kwortman@auburn.vcom.edu
Editor: Mihnea-Alexandru Găman
Student Editor: Najdat Bazarbashi
Copyeditor: Joseph Tonge & Ciara Egan
Proofreader: Ciara Egan
Layout Editor: Francisco J. Bonilla-Escobar
Process: Peer-reviewed
Cite as: Wortman II KO, Wortman Sr KO. Pneumatocele-Induced Pneumothorax in a Patient with
Post-COVID-19 Pneumonitis. A Case Report. Int J Med Students. 2021 Jul-Sep;9(3):223-6.
Copyright © 2021 Kevin O. Wortman II, Kevin O. Wortman Sr.
This work is licensed under a Creative Commons Attribution 4.0 International License.
International Journal of Medical Students, VOLUME 9, NUMBER 3, September 2021


